What Are The Symptoms Of Thyroid Cancer
The earliest sign of thyroid cancer is typically a lump or nodule at the base of the neck. You may be able to see and feel this lump yourself, or your physician may notice it during a routine checkup. Other symptoms of thyroid cancer that may be present early on before it has metastasized include:
- Changes in your voice or constant hoarseness
- Pain or soreness in the front of the neck
- A persistent cough
- Trouble swallowing
- Difficulty breathing
When thyroid cancer advances and metastasizes to distant areas of the body, some additional symptoms may be present. Metastatic thyroid cancer symptoms include:
Signs And Symptoms Of Advanced Medullary Thyroid Cancer
5 percent of thyroid cancer diagnoses. Detecting the cancer early can be difficult.
Medullary thyroid cancer commonly advances from the thyroid into the lymph nodes. Undiagnosed medullary thyroid cancer can spread into other neck tissues and eventually reach the liver, lungs, bone, and brain. Once it reaches distant parts of the body its unlikely to be cured.
Clinical Symptoms And Diagnosis Of Lung Metastases
Among all 47 patients, 4 were diagnosed based on Criterion 1, 19 were diagnosed based on Criterion 2, 3 were diagnosed based on Criterion 3, and 21 were diagnosed according to Criterion 4 One patient had synchronous bone and lung metastases, and three patients had synchronous lung and mediastinal metastases. Thirteen patients had locoregional recurrent disease without undergoing surgical resection of these 13 patients, 10 had a solitary lymph node metastasis, the size of which stabilized during follow-up, and the patients were unwilling to undergo surgery. The remaining three patients had locally invasive lesions that could not be surgically resected. Forty-three patients with lung metastases were asymptomatic, while four had clinical symptoms related to the lung metastatic lesions: breathing difficulty in one, hemoptysis in one, and dry cough in two.
Also Check: Natural Cures For Thyroid Disorders
Whole Brain Radiation Therapy
Ten patients received whole brain radiation therapy in our series, at doses ranging from 3054 Grays over 1030 treatments, with or without boost to the tumor bed. Of these patients, three had radiation given in the adjuvant setting and one in the neoadjuvant setting these patients were not considered assessable for response. In addition, two patients were treated in the preterminal disease setting and did not undergo reimaging after treatment. Of the remaining four patients who underwent reimaging after treatment and therefore were assessable for response, three were noted to have regression of their brain metastases whereas one patient had stable disease, although this assessment was performed on the last day of radiation treatment because of a change in the patients mental status during clinical deterioration.
For those patients who received whole brain radiation therapy, the overall survival from the time of diagnosis of brain metastasis was 9.5 months . For those patients who did not receive whole brain external bean radiation therapy, survival was 27.0 months . As stated earlier, two of the treated patients were considered to have terminal disease. However, eliminating these patients from the calculation increased the survival of the treated patients to only 10.8 months.
Evaluation Of Changes In Chest Ct Images

Chest CT responses were assessed using Response Evaluation Criteria in Solid Tumors as follows: i) complete response , disappearance of all lesions ii) partial response , 30% decrease in the sum of lesions diameters, taking as reference the baseline sum diameters iii) progressive disease , 20% increase in the sum of lesion diameters or appearance of greater than or equal to one new lesions is also considered progression and iv) stable disease , neither sufficient shrinkage to qualify for PR nor sufficient increase to qualify for PD.
Also Check: Can T Lose Weight Thyroid
Evaluation Of Changes In Serum Tg Level
After at least two courses of 131I therapy, changes in Tg level were classified into three types: effectiveness ), stabilization and ineffectiveness according to our previously study . i) Effectiveness: compared with pretreatment, the serum Tg levels exhibited a reduction of 25% ii) stabilization: compared with pretreatment, the serum Tg decreased or increased by < 25% and iii) ineffectiveness: compared with pretreatment, the serum Tg increased by 25%.
Tests That May Be Done
Blood tests: Blood tests alone cant tell if a thyroid lump is cancer. But they can help show if the thyroid is working the way it should.
Ultrasound: For this test, a small wand is moved over the skin in front of your neck. It gives off sound waves and picks up the echoes as they bounce off the thyroid gland. The echoes are made into a picture on a computer screen. How a lump looks on ultrasound can sometimes help tell if its cancer, but ultrasound cant tell for sure.
Radioiodine scan: For this test, a low dose of radioactive iodine is swallowed or put into a vein. Over time, the iodine is absorbed by the thyroid gland. A special camera is then used to see the radioactivity. Nodules that have less iodine than the rest of the thyroid can sometimes be cancer.
CT or CAT scan: Its a special kind of x-ray that takes detailed pictures of the thyroid and can show if the cancer has spread.
MRI scan: This test uses radio waves and strong magnets instead of x-rays to take pictures. MRI scans can be used to look for cancer in the thyroid, or cancer that has spread.
PET scan: In this test, you are given a special type of sugar that can be seen inside your body with a camera. If there is cancer, this sugar shows up as hot spots where the cancer is found. This test can be very useful if your thyroid cancer is one that doesnt take up radioactive iodine.
Thyroid biopsy
If the diagnosis is not clear after an FNA biopsy, you might need another kind of biopsy to get more cells to test.
Read Also: Side Effects Of Thyroid Meds
What Is The Thyroid
It’s a butterfly-shaped gland in your neck that makes hormones that go into your blood and then to every cell in your body. Thyroid hormones play a big role in helping your body work right. They help keep you warm and give you energy. They also support your muscles as well as your heart, brain, and other organs.
Papillary And Follicular Thyroid Cancer Stage Iv
If you are at stage IV, it means the cancer has spread. Your doctor assigns the letters âA,â âBâ and âCâ to show how far.
- Stage IVA — The cancer has spread beyond your thyroid. It now is under your skin, or it affects your larynx, esophagus or trachea. A smaller tumor in more distant lymph nodes is also considered stage IVA.
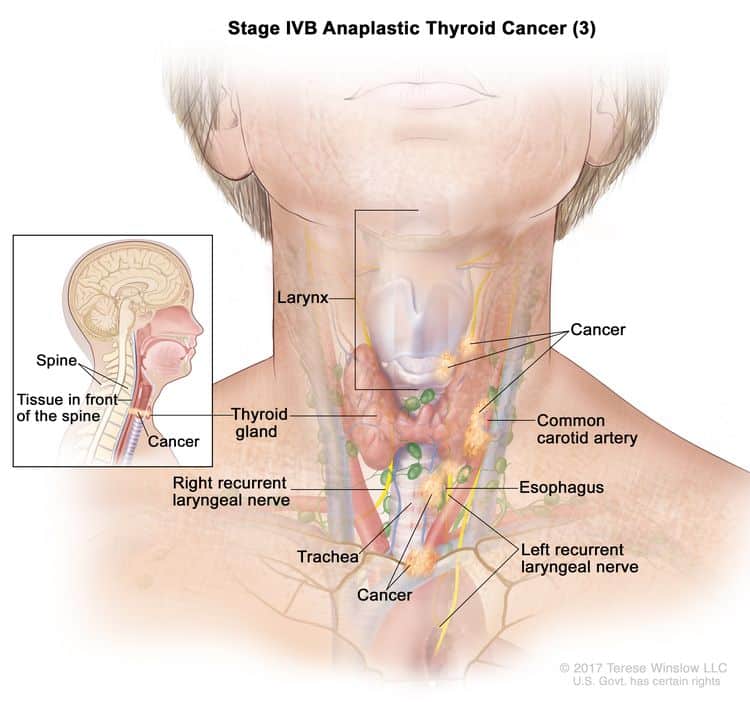
- Stage IVB — The tumor has grown toward your spine or into nearby large blood vessels, like the carotid arteries. These carry blood to your brain, face, and neck. It might have also spread to your lymph nodes.
- Stage IVC — The cancer has spread beyond the thyroid, and to distant sites of the body. It may be in your lungs, bones, and lymph nodes.
Recommended Reading: Treating Thyroid Cancer Without Surgery
Differentiated Thyroid Cancer In Patients Younger Than 55
Younger people have a low likelihood of dying from differentiated thyroid cancer. The TNM stage groupings for these cancers take this fact into account. So, all people younger than 55 years with these cancers are stage I if they have no distant spread and stage II if they have distant spread. This table includes patients 55 or older as well as younger than 55.
|
AJCC Stage |
|
|
Any N |
The cancer is any size and might or might not have spread to nearby lymph nodes . It has spread to other parts of the body, such as distant lymph nodes, internal organs, bones, etc. . |
* The following additional categories are not listed on the table above:
- TX: Main tumor cannot be assessed due to lack of information.
- T0: No evidence of a primary tumor. The N categories are described in the table above, except for:
- NX: Regional lymph nodes cannot be assessed due to lack of information.
Positron Emission Tomography /ct Scan
This shows a PET/CT scan of a patient with recurrent papillary thyroid cancer.
PET/CT scan of a patient with recurrent papillary thyroid cancer. The patient had already undergone three surgeries to treat cancer. The bright orange circle on the left is a lymph node where the papillary thyroid cancer has spread. The black area to the left of the bright spot is the lungs. This view of thyroid cancer with metastatic lymph node involvement is located next to the trachea, which should only be removed by a highly skilled surgeon. It will take about 15 minutes with a nearly 98% chance that it will never recur.
Also Check: What Are The Risk Factors For Thyroid Cancer
Cancer May Spread From Where It Began To Other Parts Of The Body
When cancer spreads to another part of the body, it is called metastasis. Cancer cells break away from where they began and travel through the lymph system or blood.
- Lymph system. The cancer gets into the lymph system, travels through the lymph vessels, and forms a tumor in another part of the body.
- Blood. The cancer gets into the blood, travels through the blood vessels, and forms a tumor in another part of the body.
The metastatic tumor is the same type of cancer as the primary tumor. For example, if thyroid cancer spreads to the lung, the cancer cells in the lung are actually thyroid cancer cells. The disease is metastatic thyroid cancer, not lung cancer.
Recommended Reading: Castor Oil Pack For Thyroid
Diagnostic Criteria For Dtc Pulmonary Metastases

Definitive cytological or pathologic confirmation was not possible in all patients therefore, diagnosis of pulmonary metastases was based on clinical and postoperative or follow-up chest CT findings, diagnostic or therapeutic 131I whole-body scan and serum Tg levels. A patient satisfying the following criteria was considered to have pulmonary metastases: i) pathological results confirmed ii) pulmonary 131I uptake on 131I-WBS+pulmonary node on chest CT+elevated serum Tg level iii) pulmonary 131I uptake on 131I-WBS+normal chest CT+elevated serum Tg level or iv) no pulmonary 131I uptake on 131I-WBS+pulmonary nodes on chest CT+elevated serum Tg level.
According to the results of 131I-WBS, pulmonary metastases were classified as 131I-avid and non-131I-avid . According to the chest CT results, patients were divided into three categories: i) included patients with negative chest CT but 131I uptake on 131I-WBS, defined as fine miliaric ii) included patients with micronodular pulmonary metastases, defined radiologically as 1cm in diameter and iii) included patients who had macronodular pulmonary metastases, defined radiologically as > 1cm in diameter. According to the discovery time, pulmonary metastases were defined as initial and developed .
Also Check: Is Vitamin C Good For Thyroid Patients
How Quickly Does Anaplastic Thyroid Cancer Develop
Anaplastic thyroid cancer is one of the most aggressive and fastest-growing types of cancer. It can grow and spread rapidly in a matter of weeks.
About 50% of people with ATC have metastasis in distant areas of their body at diagnosis. The most common sites of distant metastasis in ATC are your lungs, bones and brain.
What Will Happen After Treatment
Most people do very well after treatment, but you may need follow-up care for the rest of your life. This is because most thyroid cancers grow slowly and can come back even 10 to 20 years after treatment. Your cancer care team will tell you what tests you need and how often they should be done.
Be sure to go to all of these follow-up visits. You will have exams, blood tests, and maybe other tests to see if the cancer has come back. At first, your visits may be every 3 to 6 months. Then, the longer youre cancer-free, the less often the visits are needed.
Sometimes treatments may not cure your cancer. You many need to keep getting treatment and care. From time to time tests will be done to see how your treatment is working.
Having cancer and dealing with treatment can be hard, but it can also be a time to look at your life in new ways. Call us at 1-800-227-2345 or talk to your cancer care team to find out what you can do to feel better.
You cant change the fact that you have cancer. What you can change is how you live the rest of your life.
You May Like: Best Doctor For Thyroid Surgery
Characteristics Of Patients With Pulmonary Metastases
There were 372 enrolled patients with a predominance of females . The ratio was lower than that observed in the general series of DTC patients, which means that pulmonary metastases are relatively more frequent in male patients. The mean age at diagnosis was 54.25±16.08 years and the mean follow-up period was 59.48±40.41 months. The initial pulmonary metastases were detected in 43 patients and the remaining 329 patients were diagnosed at follow-up . Chest CT showed that pulmonary metastases were negative in 28 patients, micronodular in 313 patients and macronodular in 31 patients. 131I-avid pulmonary metastases was observed in 256 patients and non-131I-avid pulmonary metastases was found in 116 patients. The median cumulative radioiodine dose was 18.315GBq with a range of 3.786.95GBq . A single dose was given to 37 patients, two doses to 61 patients and greater than or equal to three doses to the remaining 274 patients.
Questions To Ask The Doctor
- What treatment do you think is best for me?
- Whats the goal of this treatment? Do you think it could cure the cancer?
- Will this treatment affect my ability to have children? Do I need to avoid pregnancy for a while?
- Will treatment include surgery? If so, who will do the surgery?
- What will the surgery be like?
- Will I need other types of treatment, too? Whats the goal of these treatments?
- What side effects could I have from these treatments?
- What can I do about side effects that I might have?
- Is there a clinical trial that might be right for me?
- What about special vitamins or diets that friends tell me about? How will I know if they are safe?
- How soon do I need to start treatment?
- What should I do to be ready for treatment?
- Is there anything I can do to help the treatment work better?
- Whats the next step?
Recommended Reading: How Can I Get Armour Thyroid
What Are The Symptoms Of Papillary Thyroid Cancer
The main sign of papillary thyroid cancer is a painless lump or nodule on your thyroid gland. PTC usually doesnt cause any other symptoms.
In rare cases, you may experience pain in your neck, jaw or ear from PTC. If the nodule is large enough to compress your windpipe or esophagus, it may cause difficulty with breathing or swallowing.
Demographic And Histopathological Features
Of the 110 patients with pediatric DTC, 21 had lung metastases. One patient was lost to follow-up after he had undergone total thyroidectomy and had received the first dose of I-131 and excluded from further analysis. The other 20 patients included 4 males and 16 females , with a median age of 14.5 years . The main demographic and histopathological features of these patients with lung metastases and those without evidence of distant metastases are summarized in . None of the patients had a history of head and neck irradiation. None of the patients had a family history of known hereditary syndromes associated with an increased risk of DTC . However, one patient had a family history of TC in her mother . The median tumor size was 5 cm . The rates of tumor multifocality , bilaterality , extrathyroidal extension , lymphovascular invasion , and LN metastases were high, consistent with the invasive nature of these metastatic tumors.
You May Like: Are Home Thyroid Tests Accurate
Papillary Thyroid Cancer Overview
Papillary thyroid cancer is the most common of all thyroid cancers . It can also be called papillary thyroid carcinoma since carcinoma implies a certain type of cancer. Since thyroid cancer is relatively common, and papillary thyroid cancer is the most common form of thyroid cancer, it is very likely that you will know somebody that had or has this form of cancer. Papillary thyroid cancer typically starts within the thyroid as growth, or bump on the thyroid that grows out of the otherwise normal thyroid tissue. Papillary thyroid cancer is clearly increasing in its incidence both in the United States and globallyit is one of the few cancers that are becoming more common, but we dont know why this is happening. Our Introduction to Thyroid Cancer page has a great general overview of all types of thyroid cancerread it if you havent already!
I Treatment Of Lung Metastasis
At 16 months after total or near-total thyroidectomy combined with neck lymph node dissection, the standard 131I treatment at our institution was performed in these patients with PTC. Before 131I treatment, each patient was given a low-iodine diet and began levothyroxine withdrawal for at least 2 weeks to achieve a TSH level of 30 mIU/L. The patients underwent routine measurements of free triiodothyronine , free thyroxine , TSH, Tg, and TgAb neck ultrasonography and CT scans before oral administration of 131I treatment. We subsequently used an empirical active regimen to determine the prescribed activity of 131I. Specifically, 3.7 GBq was taken orally for the first time to ablate thyroid remnants oral doses of 131I with a standard activity of 5.557.40 GBq were used for subsequent treatment of lung metastases of PTC. At 47 days after 131I oral administration, 131I-WBS and/or 131I-SPECT/CT fusion imaging was performed for these patients. The repeated 131I treatment was suspended in patients with non-131I-avid lung metastases on the 131I-WBS after completion of residual thyroid tissue ablation.
Recommended Reading: Where Does Thyroid Cancer Usually Metastasize To