When I Got Home I Started Googling Bug Eyes And Droopy Eyelids
Thats when I found out about Graves eye disease, also known as thyroid eye disease . As I learned, puffy eyelids, a gritty feeling in your eyes, and bulging eyes could all be due to swelling from an abnormal immune reaction to the muscles and fatty tissue around my eyes.
While its not a given when youre diagnosed with Graves disease that youll develop TED, up to 50 percent of people with Graves disease have eye symptoms, most often within six months of their diagnosis, according to the American Thyroid Association. This may be because the same out-of-whack antibody that attacks your thyroid can also target your eyes.
I suspected that this was what was going on with me, so I went to an optometrist that spring and asked for a referral to an eye doctor who worked with TED patients. He ignored my requests, but I walked out with a new pair of glasses.
After more research online, I found an eye doctor and surgeon near me who worked with TED patients. At my first appointment, the doctor told me he wasnt sure if I had TED, and if I did, it was a mild case. He advised that I schedule a follow-up appointment in six months.
When I went back in, they told me there was nothing they could do to help with my swollen eyelids or bulging eyesId just have to live with them. I left completely devastated and cried all the way home.
Who Is At Risk For Thyroid Eye Disease
Thyroid eye disease is most commonly associated with Graves disease. It can also occur with normal thyroid hormone levels or low levels of thyroid hormones .
Other risk factors for thyroid eye disease include:
- Age: Usually affects middle-age adults but can occur at any age
- Gender: Females are affected more than males
- Family history of thyroid eye disease
- Smoking: Smoking increases the risk of thyroid eye disease by 78 times, causes thyroid eye disease to have a longer active phase, and it reduces the effectiveness of treatments
- Radioactive iodine therapy: Radioactive iodine has been used to treat hyperthyroidism and Graves disease. This treatment should be used with caution in people with active thyroid eye disease as it may worsen the condition unless steroids are given at the same time
- Low blood levels of selenium, a dietary mineral.
Table 1 Tao Evaluation
- Intraocular pressure
- Adnexal examination
- Orbital ultrasound to assess extraocular muscle size
- Orbital CT without contrast or MRI to assess extraocular muscle size, orbital fat and proptosis
You can make the diagnosis of TAO based on presenting ocular signs and symptoms. Changes in appearance and exposure symptoms are the most common early findings in TAO.9 Other symptoms are vague and often attributed to normal aging, especially in middle-aged women with eyelid swelling that is worse in the morning.12
The most common sign in TAO is lid retraction, which occurs in 82% of patients.13 This may be due to increased sympathetic tone, overaction of the levator and superior rectus muscles to compensate for inferior rectus restriction, or inflammation and scarring of the levator complex .
The second most common sign is proptosis , which is caused by expansion of the orbital fat, muscles or both . Proptosis can be measured with an exophthalmometer. Values greater than 18mm to 20mm for Caucasians, 16mm to 18mm for Asians and 20mm to 22mm for African-Americans suggest proptosis. Asymmetry of 2mm or greater also suggests proptosis.14,15 If a clinician does not have an exophthalmometer, orbital CT scans can evaluate the amount of proptosis as well.
| Fig. 3. Upper eyelid retraction and proptosis in a patient with orbital congestion in the active phase. |
Don’t Miss: How Do You Check Your Thyroid Function
Deterrence And Patient Education
All patients with thyroid disorders should be routinely screened for early signs of thyroid eye disease. Regular follow-up of asymptomatic GD and mild TED cases can help prompt diagnosis and management of sight-threatening complications. The patients should be explained the early signs of DON – altered color vision, diminished contrast sensitivity, decreased field of vision, and decreased visual acuity.
Pearls And Other Issues
A high index of suspicion is essential for patients with the classic symptoms of thyroid eye disease, with no history of thyroid disorders or a euthyroid status at presentation. An endocrine workup and orbital imaging are essential for a definite diagnosis in the absence of classical clinical presentation.
The management includes strict maintenance of euthyroid status, cessation of smoking, adequate lubrication, adequate control of the IOP, and monitoring of disease progression as per the CAS / VISA scoring systems at regular follow-ups. Any sign of progression to active disease or sight-threatening disease warrants urgent management.
Don’t Miss: Can Thyroid Issues Cause Erectile Dysfunction
Imaging Studies For Diagnosing Go And Defining Disease Activity
Imaging studies can be helpful in establishing the diagnosis of GO because they provide objective morphological findings of the orbital structures. Based on such studies , it is possible to establish the degree of extraocular muscle and orbital fat enlargement, exclude coexisting orbital pathology, clarify a confusing clinical picture, and perform surgical planning . A CT scan with positive findings is included in many sets of diagnostic criteria for GO ,.
GO presents an unusual imaging pattern. The extraocular muscles appear to be the primary area of orbital involvement. Despite attempts to establish normative measurements , the assessment of muscle enlargement is often subjective and requires comparison with the opposite orbit or prior qualitative experience. Patients with GO usually present symmetrical, multiple extraocular muscle enlargement in both orbits, although asymmetrical muscle involvement can occur. However, true unilateral orbital involvement is uncommon, occurring in only 6 to 10% of patients . The muscles most frequently affected are the medial and inferior recti .
Coronal CT scans from two patients with Graves’ orbitopathy. A) Patient with symmetric enlargement of the extraocular muscles in both orbits. B) Patient with asymmetric involvement of the extraocular muscles.
Impact Of Thyroid Eye Disease And Photos
I think its hard for loved ones to grasp just how impactful not recognizing yourself in pictures is and how damaging it can be to self-esteem and mental health. Comments like Were your friends, we dont care what you look like! and Youll have surgery and everything will be fine! though well-intended felt dismissive and diminished the true emotional trauma I was going through. But on two occasions I felt seen. Oh lets take a fun group photo with sunglasses! She looked at me, leaned in, and whispered, Is that okay? Ive been listening. And a tear came to my eye. I eventually came to accept that it was okay to not take pictures for a while. It was better for my mental health and overall well-being, though I was always game for group sunglass photos.
Im happy to say that I finally had orbital decompression surgery a few weeks ago. As I wait for the internal swelling to go down and for my upcoming lid surgery, I cant help but have a million questions – What will my eyes look like? I know it wont be exactly the same as it was before, but will I look more like me? Will I have to re-learn how to tilt my head and smile for the camera? Will I feel comfortable in photos again? I have hope.
Also Check: Blood Test For Thyroid Levels
Table 3 Management Of Thyroid Eye Disease
Disease Stage Refractory
- Steroid-sparing immunomodulators
When using CAS, note that severe disease complications, such as dysthyroid optic neuropathy, are still possible with low CAS scores, and patients with high CAS scores may have long-standing congestive changes that are unresponsive to any immunotherapy, requiring mechanical surgical decompression.
Latent. After the active phase plateaus, the patient enters the quiescent burn-out phase. This latent, chronic fibrotic phase presents with similar clinical findings as the active inflammatory phase but does not have many of the inflammatory signs seen during the active phase .23 These patients require frequent follow-up, as reactivation of inflammation can occur in 5% to 10% of patients over their lifetime.24
You May Notice The Following Appearance And Vision Changes:
- Misaligned eyes or eyes that dont work together
- Sensitivity to light
- Eye pain and pressure
The changes caused by TED may also affect your emotions, making you feel anxious or depressed.
Learn more about the symptoms and signs of TED as well as the impact it can have on your emotional well-being.
While the length of the acute phase of TED is different for everyone, it usually lasts between 6 months to 3 years. During this time, symptoms can change or continue to get worse. Ideally, treatment should be given during the acute phase.
Recommended Reading: What Are The Tests For Thyroid Function
In March Of 2017 About Four Months After My Graves’ Disease Diagnosis I Was Starting To Feel Better But I Began To See Subtle Changes In My Eyes
One morning, I noticed that my upper eyelids were swollen and my eyes were red. Although I didnt typically have seasonal allergies that time of year, I thought that was the most likely culprit, so I took some over-the-counter allergy meds. That seemed to help with the redness a little.
My eyes also felt tired and gritty, and if I rubbed them, my right eye would get broken blood vessels. But a friend assured me that this was normal, telling me it happened to her sometimes, too.
Following Treatment Guidelines For Graves’ Disease And Hyperthyroidism
Not receiving treatment for Graves disease and hyperthyroidism makes you more likely to develop problems with your eyes. In addition, taking your medications correctly for Graves disease and hyperthyroidism can affect the condition of your eyes.
Other lifestyle factors that may affect thyroid eye disease development include:
- Changes in hormones
- Taking certain medications, such as amiodarone for heart disease
- Not having enough or having too much dietary iodine
Also Check: Treatment For Thyroid Cancer That Has Spread To Lungs
What Are The Symptoms Of Thyroid Eye Disease
If you have Graves disease, eye symptoms most often begin within six months of disease diagnosis. Very rarely, eye problems may develop long after the Graves disease has been treated. In some patients with eye symptoms, hyperthyroidism never develops and, rarely, patients may have hypothyroidism. The severity of the eye symptoms is not related to the severity of the hyperthyroidism.
Symptoms of thyroid eye disease are caused by the tissues, fat, and muscles of the eye socket swelling and pushing the eyeball forward. It may be possible that symptoms may appear in one eye more than the other. The symptoms of thyroid eye disease include:
Dry, gritty and irritated eyes
Red eyes
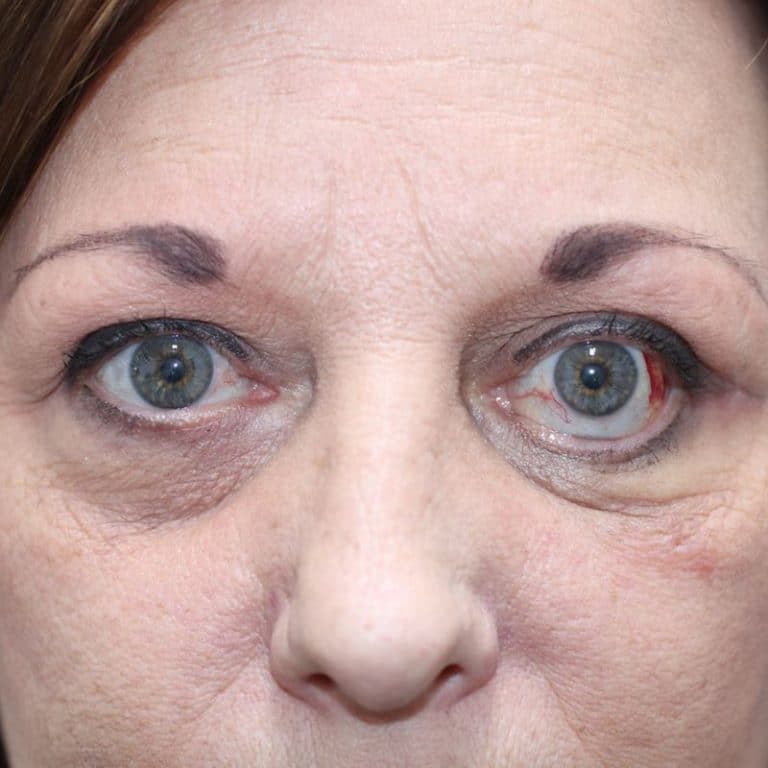
Bulging eyes and lid retraction giving a staring or startled appearance
In more advanced thyroid eye disease, there may also be:
- Trouble moving eyes and closing eyes
- Inability to completely close your eye causing a corneal ulcer
- Colors appear to be dull or not as bright
- Blurred or loss of vision due to optic nerve compression or corneal damage
Double vision
The Thyroid Gland And Important Terms
Thyroid Gland: The thyroid gland is located in the front of your neck. It produces thyroid hormones that are sent to the blood and carried around to other parts of your body. These hormones help your body use energy, stay warm and keep the brain, heart, muscles, and other organs working normally. The thyroid gland can become overactive or underactive . This is most often due to an autoimmune disease in your body.
Hyperthyroidism: Hyperthyroidism is a condition where the thyroid gland is stimulated by the immune system to produce more thyroid hormones than are needed by the body. Symptoms may include weight loss, nervousness, irritability, increased perspiration, fast heart rate, hand tremors, difficulty sleeping, thinning of the skin, brittle hair, and frequent bowel movements.
Hypothyroidism: Hypothyroidism is a condition where thyroid gland function is blocked by the immune system and not enough thyroid hormone is produced for the bodys needs. Symptoms may include feeling cold and tired, having drier skin, becoming forgetful and depressed, and having constipation.
Autoimmune disease: If you have an autoimmune disease, your immune system mistakenly attacks your body. Autoimmune diseases can affect many parts of the body. The cause of autoimmune diseases is largely unknown.
The Thyroid Gland
You May Like: What Happens If Thyroid Cancer Goes Untreated
Treatment Of Thyroid Eye Disease
For a mild case, use lubricating eye drops and artificial tears a few times during the day. Avoid wind and bright light.
If you have severe symptoms, your healthcare provider may prescribe corticosteroids such as prednisone to reduce swelling. In a very small percentage of patients, orbital decompression surgery may be recommended.
This procedure removes the bone between the eye socket and the air sinus behind it so your eye has more room. This can improve your vision but there is a risk of double vision.
Double vision can also occur when scar tissue from the ophthalmopathy makes an eye muscle too short. Eye muscle surgery can be used to attach the muscle at a point where it will again be the correct length to provide single vision. However, more than one surgery may be needed to be successful.
Table 2 Clinical Activity Score
Retrobulbar pain 0-2: inactive TAO3-7: active TAO
The VISA classificationVision, Inflammation, Strabismus and Appearancewas developed to permit grading of both clinical severity and activity based on both subjective and objective inputs .20 This system helps direct appropriate management in a logical sequence by targeting the most relevant aspect of the disease affecting the patient. For example, vision dysfunction from the optic nerve is the first priority. VISA is also beneficial in assessing TAO and grading changes and can act as a guide for therapy.20 The International Thyroid Disease Society has adopted it, and it is used in recent clinical trials.
Another popular method grades TAO from mild to severe.21 The European Group on Graves Orbitopathy defines mild disease as minimal eyelid swelling, lid retraction or proptosis with little or no extraocular muscle dysfunction. Moderate to severe TAO consists of some form of active disease with or without ocular motility dysfunction with diplopia and inflammatory features interfering with the ability to function. It may also include significant proptosis. Serious disease refers to sight-threatening conditions such as dysthyroid optic neuropathy and corneal ulceration.9
| Fig. 5. The VISA classification form allows clinicians to monitor the severity and the activity of TAO. |
Recommended Reading: Thyroid Cancer Signs To Never Ignore
Pca Of Structural Metrics: Ted Subtypes
The 25 structural metrics obtained from CT imaging are used to perform a PCA. Figure 4 shows the factor loadings of the metrics for top 12 components that explain 97% of the variance. The top two components, which explain over 60% of the total variance, show two distinct clusters of metrics. Component 1 shows characteristics with large size and volume measurements of the extraocular muscles. Component 2 shows longer and thinner optic nerves with increased orbital fat . These two clusters of structural metrics align with Nunerys classification of TED subtypes.1214 Nunery describes a subtype of TED patients with motility defects and enlarged extraocular muscles and a subtype without motility defects and increased orbital fat . Examples of the two subtypes of segmented labels are shown in Fig. 5. However, there is a high variability in the presentation of the phenotypes in individual patients. Each individual can express either, both or none of the phenotypes to varying degrees. Figure 6 shows the distribution of patients by phenotype and sex.
Subtypes of TED. Example of subtype 1 showing big muscleswith high values along component 1. Example of subtype 2 showing longer and thinner optic nerve, and greater orbital fatwith high values along component 2.
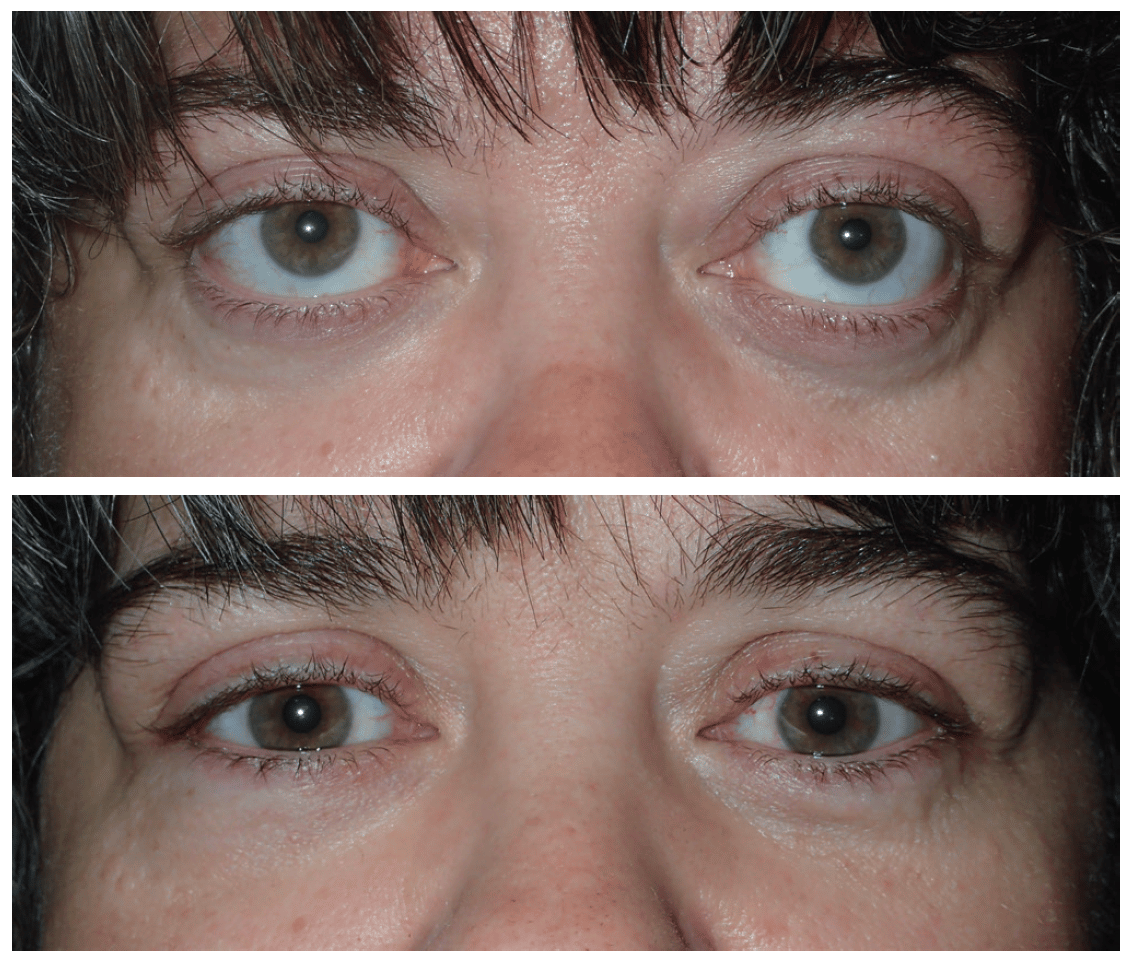
Patient Photos Of Chronic Thyroid Eye Disease Before And After Tepezza Treatment
Below are some photos that doctors have taken of real patients with chronic TED before TEPEZZA and after 8 infusions. Individual results may vary.
Before TEPEZZA
Real patient treated with TEPEZZA. Individual results may vary.
Before receiving TEPEZZA, this patient had multiple surgeries, including:
- A thyroidectomy
- Lower lid retraction repair surgeries
- Surgery to restore the appearance of her face and eyes
Despite these treatments and surgery, the patient still had eye bulging before TEPEZZA.
Before TEPEZZA
Real patient treated with TEPEZZA. Individual results may vary.
Before receiving TEPEZZA, this patient was treated with:
- Steroids taken by mouth
- Steroid injections
- Surgery to reduce eye bulging
Despite these treatments and surgery, the patient still had double vision and eye bulging before TEPEZZA.
See more real patient photos
See how TEPEZZA helped real patients reduce eye bulging and improve physical appearance.
You May Like: Hair Loss From Thyroid Disease
Overview Of Treatment Options
Corticosteroid Therapy
Corticosteroids are a mainstay of treatment in TED. The benefit derived from corticosteroid administration is due to anti-inflammatory and immunosuppressive effects. Unfortunately, a significant percentage of patients respond only partially , and recurrences upon dose reduction or cessation are not infrequent .
- Exacerbation of diabetes mellitus, hypertension, and/or osteoporosis
- Intravenous corticosteroids
- Compared to oral administration, IV is usually better tolerated and more effective .
- Compared to months of treatment with oral prednisone, IV treatment usually lasts 12 weeks , which allows for easy and early detection of “non-responders.”
- IV decreases the need for additional medical therapy.
- Additional considerations
- If prolonged high-dose treatment is anticipated, treat with calcium, vitamin D, and a proton pump inhibitor .
- Incorporate frequent monitoring of serum electrolytes, blood glucose, liver function tests , and blood pressure.
- Patients receiving cumulative doses exceeding 8 g are at risk for hepatic toxicity, electrolyte disturbances, and cardiac arrhythmias
Orbital Radiotherapy
Orbital radiotherapy has been used in the management of TED for nearly a century and can be used alone or in conjunction with corticosteroids .
- Mechanisms of action